Under 30 Minutes
Outpatient Minor Procedure
Usually Minimal to No Downtime
Insurance Coverage
Co-Pay Variable
Self-Pay Prices Available
Common Concerns
- Change in appearance of a mole
- New skin lesion has appeared
- Personal or family history of skin cancer
- Minimal scars after removal of skin cancer
- Mole has changed colors
- Skin cancer protection
Frequently Asked Questions
How are plastic surgeons involved with skin cancer?
- Identification of Skin Cancer – Skin cancers are typically discovered by either your primary care doctor, dermatologist or plastic surgeon.
- Removal of Skin Cancer – Skin cancers are found all over the body but when found on visible areas or near important structures such as the eye, nose or lip, plastic surgeons can remove these lesions with minimal deformity as possible
- Reconstruction After Removal of Skin Cancer – Skin cancers are sometimes removed or initially biopsied by primary care doctors or dermatologists. When the area cannot be closed by simple closure, plastic surgeons are able to close these areas with skin flaps or grafts.
- Melanoma — Both Dr. Ewart and Dr. Tarakji are experienced in treating and reconstructing melanoma patients. This often requires performing a sentinal lymph node dissection, to identify the first draining lymph node from the area of the melanoma.
- Minimize Scarring – Many patients request seeing a plastic surgeon to have either the initial cancer removed or the residual defect to be repaired in order to have the best result possible.
At Augusta Plastic Surgery, we have the unique ability to diagnose, treat and reconstruct any type of skin cancer you may have with the 2 ultimate goals in mind:
- Completely remove the cancer
- Most cosmetic result as possible
What are the main types of skin cancer?
There are a variety of skin cancers but these are the three most commonly seen:
- Squamous Cell Cancer
- Basal Cell Cancer
- Melanoma
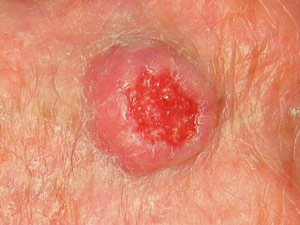
What is Basal Cell Cancer?
BCCs are abnormal, uncontrolled growths or lesions that arise in the skin’s basal cells, which line the deepest layer of the epidermis (the outermost layer of the skin). BCCs often look like open sores, red patches, pink growths, shiny bumps, or scars and are usually caused by a combination of cumulative and intense, occasional sun exposure.
BCC almost never spreads (metastasizes) beyond the original tumor site. Only in exceedingly rare cases can it spread to other parts of the body and become life-threatening. It shouldn’t be taken lightly, though: it can be disfiguring if not treated promptly.
In 2010, an estimated 2.8 million cases of BCC were diagnosed in the US, and the figures have continued to climb. In fact, BCC is the most frequently occurring form of all cancers. More than one out of every three new cancers is a skin cancer, and the vast majority are BCCs.
What to look for?
Frequently, two or more of these features are present in one tumor. In addition, BCC sometimes resembles noncancerous skin conditions such as psoriasis or eczema. Only a trained physician, such as a specialist in diseases of the skin, can decide for sure. If you observe any of the warning signs or some other worrisome change in your skin, consult your physician immediately.
- An open sore that bleeds, oozes, or crusts and remains open for a few weeks, only to heal up and then bleed again. A persistent, non–healing sore is a very common sign of an early BCC.
- A reddish patch or irritated area, frequently occurring on the face, chest, shoulders, arms, or legs. Sometimes the patch crusts. It may also itch or hurt. At other times, it persists with no discomfort.
- A shiny bump or nodule that is pearly or clear and is often pink, red, or white. The bump can also be tan, black, or brown, especially in dark-haired people, and can be confused with a normal mole.
- A pink growth with a slightly elevated rolled border and a crusted indentation in the center. As the growth slowly enlarges, tiny blood vessels may develop on the surface.
- A scar-like area that is white, yellow or waxy, and often has poorly defined borders; the skin itself appears shiny and taut. This warning sign may indicate the presence of an invasive BCC that is larger than it appears to be on the surface.
Treatment
Choice of treatment is based on the type, size, location, and depth of penetration of the tumor, the patient’s age and general health, and the likely outcome to his or her appearance.
Treatment can almost always be performed on an outpatient basis. With the various surgical techniques, a local anesthetic is commonly used. Pain or discomfort during the procedure is minimal, and pain afterwards is rare.
Excisional Surgery
Using a scalpel, the physician removes the entire growth along with a surrounding border of apparently normal skin as a safety margin. The skin around the surgical site is closed with stitches, and the tissue specimen is sent to the laboratory to verify that all cancerous cells have been removed. Cure rates are generally above 95 percent in most body areas, similar to those of curettage and electrodesiccation. A repeat excision may be necessary on a subsequent occasion if evidence of skin cancer is found in the specimen.
Cryosurgery
Tumor tissue is destroyed by freezing. Liquid nitrogen is applied to the growth with a cotton-tipped applicator or spray device, freezing it without requiring any cutting or anesthesia (though a local anesthetic can be used, since the technique often involves a modest amount of pain). The procedure may be repeated at the same session to ensure total destruction of malignant cells. The growth subsequently blisters or becomes crusted and falls off, usually within weeks. Temporary redness and swelling can occur, and in most cases, pigment may be lost at the site. Cryosurgery is effective for the most common tumors, especially superficial BCC, and is useful for patients with bleeding disorders or intolerance to anesthesia. This method is used less commonly today, and has a lower cure rate than the surgical techniques–approximately 85-90 percent, depending on the physician’s expertise.
Laser Surgery
Some lasers vaporize (ablate) the skin’s top layer to destroy lesions. Others (non-ablative lasers) penetrate the skin without removing the top layer; one such laser has been shown in some cases to treat small, superficial BCCs successfully. Laser therapy is not yet FDA-approved for BCC, but is sometimes used as a secondary therapy when other techniques are unsuccessful.
Topical Medications
These creams, gels, or solutions are used to treat limited, specific BCCs:
- Imiquimod is FDA-approved only for superficial BCCs, with cure rates generally between 80 and 90 percent. The cream is rubbed gently into the tumor five times a week for up to six weeks or longer. The first in a new class of drugs that work by stimulating the immune system, it causes the body to produce interferon, a chemical that attacks cancer.
- 5-Fluorouracil (5-FU), a chemotherapy drug approved to treat internal cancers, also has been FDA-approved for superficial BCCs, with similar cure rates to imiquimod. The liquid or cream is gently rubbed into the tumor twice a day for three to six weeks. Side effects are variable, and some patients do not experience any discomfort, but redness, irritation, and inflammation usually occur.
It is important to note that (unlike Mohs surgery and excisional surgery), curettage and electrodesiccation, radiation, cryosurgery, and topical medications all have one significant drawback in common – since no tissue is examined under the microscope, there is no way to determine how completely the tumor was removed.
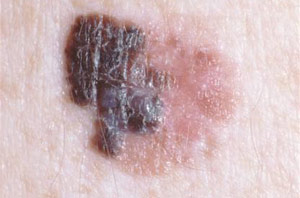
What is Melanoma?
 The most dangerous form of skin cancer, these cancerous growths develop when unrepaired DNA damage to skin cells (most often caused by ultraviolet radiation from sunshine or tanning beds) triggers mutations (genetic defects) that lead the skin cells to multiply rapidly and form malignant tumors. These tumors originate in the pigment-producing melanocytes in the basal layer of the epidermis. Melanomas often resemble moles; some develop from moles. The majority of melanomas are black or brown, but they can also be skin-colored, pink, red, purple, blue or white. Melanoma is caused mainly by intense, occasional UV exposure (frequently leading to sunburn), especially in those who are genetically predisposed to the disease. Melanoma kills an estimated 9,710 people in the US annually.
The most dangerous form of skin cancer, these cancerous growths develop when unrepaired DNA damage to skin cells (most often caused by ultraviolet radiation from sunshine or tanning beds) triggers mutations (genetic defects) that lead the skin cells to multiply rapidly and form malignant tumors. These tumors originate in the pigment-producing melanocytes in the basal layer of the epidermis. Melanomas often resemble moles; some develop from moles. The majority of melanomas are black or brown, but they can also be skin-colored, pink, red, purple, blue or white. Melanoma is caused mainly by intense, occasional UV exposure (frequently leading to sunburn), especially in those who are genetically predisposed to the disease. Melanoma kills an estimated 9,710 people in the US annually.
If melanoma is recognized and treated early, it is almost always curable, but if it is not, the cancer can advance and spread to other parts of the body, where it becomes hard to treat and can be fatal. While it is not the most common of the skin cancers, it causes the most deaths. The American Cancer Society estimates that at present, more than 120,000 new cases of melanoma in the US are diagnosed in a year. In 2014, an estimated 76,100 of these will be invasive melanomas, with about 43,890 in males and 32,210 in women.
What to look for?
Moles, brown spots and growths on the skin are usually harmless — but not always. Anyone who has more than 100 moles is at greater risk for melanoma. The first signs can appear in one or more atypical moles. That’s why it’s so important to get to know your skin very well and to recognize any changes in the moles on your body. Look for the ABCDE signs of melanoma, and if you see one or more, make an appointment with a physician immediately.
- A – Asymmetry: If you draw a line through this mole, the two halves will not match.
- B – Border: The borders of an early melanoma tend to be uneven. The edges may be scalloped or notched.
- C – Color: Having a variety of colors is another warning signal. A number of different shades of brown, tan or black could appear. A melanoma may also become red, blue or some other color.
- D – Diameter: Melanomas usually are larger in diameter than the size of the eraser on your pencil (1/4 inch or 6 mm), but they may sometimes be smaller when first detected.
- E – Evolving: Any change — in size, shape, color, elevation, or another trait, or any new symptom such as bleeding, itching or crusting — points to danger.
Treatment
The first step in treatment is the removal of the melanoma, and the standard method of doing this is by surgical excision (cutting it out). Surgery has made great advances in the past decade, and much less tissue is removed than was customary in the past. Patients do just as well after the lesser surgery, which is easier to tolerate and produces a smaller scar.
Surgical excision is also called resection, and the borders of the entire area excised are known as the margins.
Outpatient/Office Surgery
In most cases, the surgery for thin melanomas can be done as an outpatient procedure under local anesthesia. Stitches (sutures) remain in place for one to two weeks, and most patients are advised to avoid heavy exercise during this time. Scars are usually small and improve over time.
Discolorations and areas that are depressed or raised following the surgery can be concealed with cosmetics specially formulated to provide camouflage. If the melanoma is larger and requires more extensive surgery, a better cosmetic appearance can be obtained with flaps made from skin near the tumor, or with grafts of skin taken from another part of the body. For grafting, the skin is removed from areas that are normally or easily covered with clothing.
There is now a trend towards performing sentinel node biopsy and tumor removal surgery at the same time, provided the tumor is 1 mm or more thick. When the procedures are combined in this way, the patient is spared an extra visit.
Surgical excision is also called resection, and the borders of the entire area excised are known as the margins. Surgical excision is used to treat all types of skin cancer. At its best – given an experienced surgeon and a small, well-placed tumor – it offers results that are both medically and cosmetically excellent.
The physician begins by outlining the tumor with a marking pen. A “safety margin” of healthy-looking tissue will be included, because it is not possible to determine with the naked eye how far microscopic strands of tumor may have extended. The extended line of excision is drawn, so the skin may be sewn back together.
The physician will administer a local anesthetic, and then cut along the lines that were drawn. The entire procedure takes about thirty minutes for smaller lesions.
Wounds heal rapidly, usually in a week or two. Scarring depends on many factors, including the placement of the tumor and the patient’s care of the wound after the procedure.
The tissue sample will be sent to a lab, to see if any of the “safety margin” has been invaded by skin cancer. If this is the case, it is assumed that the cancer is still present, and additional surgery is required.
Setting the Margins
- In the new approach to surgery, much less of the normal skin around the tumor is removed and the margins, therefore, are much narrower than they ever were before.
- When there is an in situ melanoma, the surgeon excises 0.5-1 centimeter of the normal skin surrounding the tumor and takes off the skin layers
- down to the fat.
- In removing an invasive melanoma that is 1 mm or less in Breslow’s thickness, the margins of surrounding skin are extended to 1 cm and the excision goes through all skin layers and down to the fascia (the layer of tissue covering the muscles).
- If the melanoma is 1.01 to 2 mm thick, a margin of 1-2 cm is taken.
- If the melanoma is 2.01 mm thick or greater, a margin of 2 cm is taken.
- These margins all fall within the range of what is called “narrow” excision. When you consider that until recently, margins of 3 to 5 cm (wide excision) were standard, even for comparatively thin tumors, you can see how dramatically surgery has changed for the better. Physicians now know that even when melanomas have reached a thickness of 4 mm or more, increasing the margins beyond 2 cm does not increase survival.
Sentinal Lymph Node Biopsy
- A sentinel lymph node biopsy is a procedure that helps the doctor find out whether melanoma has spread to the lymph nodes.
- If melanoma is found during a sentinel lymph node biopsy, the doctor should remove more lymph nodes.
- Talk with your doctor about what kind of procedure is needed to evaluate and treat your melanoma and what the results will mean.
Background
Melanoma is a type of cancer that starts in color-producing cells of the skin called melanocytes. Often, but not always, melanoma develops from an existing mole. Melanoma can grow deep into the inner layers of skin and spread to the lymph nodes (tiny, bean-shaped organs that help fight infection) and other parts of the body. Treatment for melanoma is determined by the thickness (how deep the tumor has grown into the layers of the skin) of the primary tumor and whether it has spread. This is also called the stage of the cancer. Whether melanoma has spread to the lymph nodes is one of the most important factors in determining a patient’s prognosis (chance of recovery).
A sentinel lymph node biopsy (also called sentinel node biopsy or SNB) is a procedure that helps the doctor find out whether the cancer has spread to the lymph nodes. When cancer spreads from the place it started to the lymph nodes, it travels through the lymphatic system. A sentinel lymph node is the first node into which the lymphatic system drains. Because melanoma can start anywhere on the skin, the location of the sentinel lymph nodes will be different depending on where the cancer started. To find the sentinel lymph node, a harmless radioactive substance is injected as close as possible to where the melanoma started. The substance is followed to the sentinel lymph node. Then, the doctor removes one or a few of these lymph nodes to check for melanoma cells, leaving behind most of the other lymph nodes in that area.
If the biopsy results show that the cancer has not spread to the sentinel lymph node, then no additional lymph node surgery is needed. However, if melanoma is found in the sentinel lymph nodes, a lymph node dissection is usually recommended. A lymph node dissection is the surgical removal of the remaining lymph nodes in that area. The risks of a lymph node dissection vary depending on the number of lymph nodes removed during the procedure.
Recommendations
- SNB is recommended for patients with a melanoma that developed on any part of the surface of the skin and is 1 millimeter (mm) to 4 mm thick.
- SNB may be recommended to help stage and determine treatment for a melanoma that is thicker than 4 mm.
- SNB is not recommended for most patients with a thin melanoma (less than 1 mm thick), although it may be considered if the melanoma has a high risk of spreading. It is not yet certain which patients with a thin melanoma have a higher risk of the disease spreading to the lymph nodes. However, some high-risk features of melanoma include ulceration (the outer layer of skin over the melanoma is missing when viewed under a microscope) or a high mitotic rate (more cells that are dividing; a sign that the cancer may be growing rapidly).
A lymph node dissection is recommended for all patients when melanoma is found in the sentinel lymph nodes.
What This Means for Patients
For many patients with a melanoma thicker than 1 mm, SNB is a useful way to find out whether the cancer has spread from where it began. It helps your doctor plan treatment and can help you understand your prognosis. There are few side effects from the procedure, but a patient may experience infection, seroma (fluid build-up) near the surgical area, numbness, and re-opening of the surgical area. Rarely, lymphedema (build-up of lymph fluid) may occur. However, this side effect is more common for patients who have had a lymph node dissection.
If melanoma is found in the sentinel lymph nodes, a lymph node dissection to remove the remaining lymph nodes in that area allows the doctors to find out whether the cancer has spread and remove any additional lymph nodes that may contain melanoma. A patient may take longer to recover after a lymph node dissection and has a higher risk of side effects. For example, a patient who has had a lymph node dissection in the armpit or groin has a higher risk of lymphedema. However, the results of a lymph node dissection help your doctor make sure you get the appropriate treatment for your stage of melanoma. Talk with your doctor about the tests needed to diagnose melanoma and determine the stage, and how these results affect your treatment options.
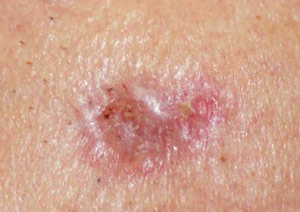
What is Squamous Cell Cancer?
Squamous cell carcinoma (SCC) is an uncontrolled growth of abnormal cells arising in the squamous cells, which compose most of the skin’s upper layers (the epidermis). SCCs often look like scaly red patches, open sores, elevated growths with a central depression, or warts; they may crust or bleed. They can become disfiguring and sometimes deadly if allowed to grow. An estimated 700,000 cases of SCC are diagnosed each year in the US, and between 3,900 and 8,800 people died from the disease in the US in 2012. Incidence of the disease has increased up to 200 percent in the past three decades in the US.
SCC is mainly caused by cumulative ultraviolet (UV) exposure over the course of a lifetime; daily year-round exposure to the sun’s UV light, intense exposure in the summer months, and the UV produced by tanning beds all add to the damage that can lead to SCC.
SCCs may occur on all areas of the body including the mucous membranes and genitals, but are most common in areas frequently exposed to the sun, such as the rim of the ear, lower lip, face, balding scalp, neck, hands, arms and legs. Often the skin in these areas reveals telltale signs of sun damage, including wrinkles, pigment changes, freckles, “age spots,” loss of elasticity, and broken blood vessels.
What to look for?
Squamous cell carcinomas typically appear as persistent, thick, rough, scaly patches that can bleed if bumped, scratched or scraped. They often look like warts and sometimes appear as open sores with a raised border and a crusted surface.
In addition to the signs of SCC shown here, any change in a preexisting skin growth, such as an open sore that fails to heal, or the development of a new growth, should prompt an immediate visit to a physician.
Treatment Options
Squamous cell carcinomas detected at an early stage and removed promptly are almost always curable and cause minimal damage. However, left untreated, they eventually penetrate the underlying tissues and can become disfiguring. A small percentage even metastasize to local lymph nodes, distant tissues, and organs and can become fatal. Therefore, any suspicious growth should be seen by a physician without delay. A tissue sample (biopsy) will be examined under a microscope to arrive at a diagnosis. If tumor cells are present, treatment is required.
Fortunately, there are several effective ways to eradicate squamous cell carcinoma. The choice of treatment is based on the tumor’s type, size, location, and depth of penetration, as well as the patient’s age and general health.
Treatment can almost always be performed on an outpatient basis. A local anesthetic is used during most surgical procedures. Pain or discomfort is usually minimal, and there is rarely much pain afterwards.
- Excision: The physician uses a scalpel to remove the entire growth, along with a surrounding border of apparently normal skin as a safety margin. The wound around the surgical site is then closed with sutures (stitches). The excised tissue specimen is then sent to the laboratory for microscopic examination to verify that all cancerous cells have been removed. A repeat excision may be necessary on a subsequent occasion if evidence of skin cancer is found in the specimen. The accepted cure rate for primary tumors with this technique is about 92 percent. This rate drops to 77 percent for recurrent squamous cell carcinomas.
- Cryotherapy: The physician destroys the tumor tissue by freezing it with liquid nitrogen, using a cotton-tipped applicator or spray device. There is no cutting or bleeding, and no anesthesia is required. The procedure may be repeated several times at the same session to help ensure destruction of all malignant cells. The growth becomes crusted and scabbed, and usually falls off within weeks. Redness, swelling, blistering and crusting can occur following treatment, and in dark-skinned patients, some pigment may be lost. Inexpensive and easy to administer, cryosurgery may be the treatment of choice for patients with bleeding disorders or intolerance to anesthesia. However, it has a lower overall cure rate than the surgical methods. Depending on the physician’s expertise, the 5-year cure rate can be quite high with selected, generally superficial squamous cell carcinoma; but cryosurgery is not often used today for invasive SCC because deeper portions of the tumor may be missed and because scar tissue at the cryotherapy site might obscure a recurrence.
- Topical: 5-fluorouracil (5-FU) and imiquimod, both FDA-approved for treatment of actinic keratoses and superficial basal cell carcinomas, are also being tested for the treatment of some superficial squamous cell carcinomas. Successful treatment of Bowen’s disease, a noninvasive SCC, has been reported. However, invasive SCC should not be treated with 5-FU. Some trials have shown that imiquimod may be effective with certain invasive SCCs, but it is not yet FDA-approved for this purpose. Imiquimod stimulates the immune system to produce interferon, a chemical that attacks cancerous and precancerous cells, while 5-FU is a topical form of chemotherapy that has a direct toxic effect on cancerous cells.
Because most treatment options involve cutting, some scarring from the tumor removal should be expected. This is most often cosmetically acceptable with small cancers, but removal of a larger tumor often requires reconstructive surgery, involving a skin graft or flap to cover the defect. .
Squamous cell carcinomas usually remain confined to the epidermis (the top skin layer) for some time. However, the larger these tumors grow, the more extensive the treatment needed. They eventually penetrate the underlying tissues, which can lead to major disfigurement, sometimes even the loss of a nose, eye or ear. A small percentage spread (metastasize) to distant tissues and organs. When this happens, squamous cell carcinomas frequently can be life-threatening.
Metastases most often arise on sites of chronic inflammatory skin conditions and on the ear, nose, lip, and mucosal regions, including the mouth, nostrils, genitals, anus, and the lining of the internal organs.